- Your cart is empty
- Continue Shopping
An Overview of Cellulitis
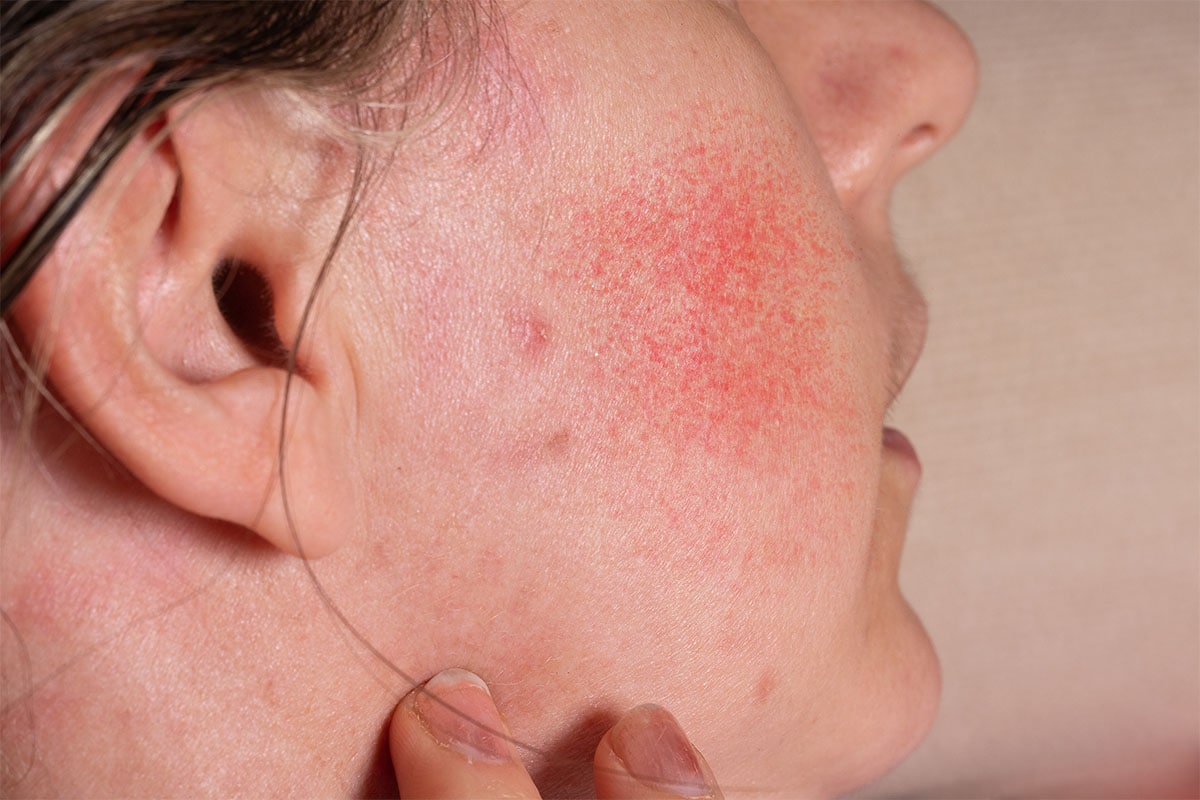
With over 14 million cases reported in the United States alone, cellulitis is one of the most common skin conditions. The most common site of cellulitis is located on the lower extremity.
Although a prevailing skin condition, cellulitis is often treated in an outpatient setting with a non-invasive approach. Like many health conditions, however, cellulitis can become severe if left untreated and can lead to severe illness. Yet, with proper treatment, it can be managed quickly and effectively.
What follows will be an overview of cellulitis, its signs and symptoms, causes and risk factors, and available treatment and prevention mechanisms.
Characteristics of Cellulitis
Cellulitis is defined as a common bacterial skin infection that leads to rashes, redness, and pain at the source of the condition. The infection occurs at the outermost level of the skin. Cellulitis should not be confused with other common skin conditions such as dermatitis, phlebitis, or necrotizing fasciitis. The most common types of bacteria that cause cellulitis are staphylococcus and streptococcus type bacteria.
Cellulitis can often be caused by bacteria such as MRSA, which can be a difficult infection to manage. MRSA, or Methicillin-Resistant Staphylococcus Aureus, is a type of staph infection known for its resistance to treatment. MRSA contraction is quite high in the hospital setting and requires intense methods to try to control these infection rates. MRSA is also very prevalent in the community and results from injuries to the skin, use of recreational IV Drugs, cosmetic shaving, and shared use of contaminated clothing. It can also be transferred from animals.
Necrotizing fasciitis is another rare bacterial infection involving the deepest layers of the skin where the fascia is located. The fact that the infection is located at such a deep layer is why this infection is so difficult to treat.
Most cases of cellulitis are self-contained, and recovery from the condition usually occurs within 7-10 days after appropriate antibiotic treatment. In more minor cases, cellulitis may be able to be managed without additional medication. Yet, in severe cases of cellulitis, patients may require more invasive care.
In rare circumstances, untreated cellulitis can advance to severe infection that spreads throughout the body and bloodstream in a condition known as sepsis, and this is a life-threatening condition.
Signs and Symptoms of Cellulitis
The signs and symptoms of cellulitis can vary based on the location of the infection and the type of bacteria involved. Many times the infection can be painful, but, for example, cellulitis located on the foot will likely be more painful than cellulitis located on the forearm. The area of infection usually has characteristic signs of redness and swelling.
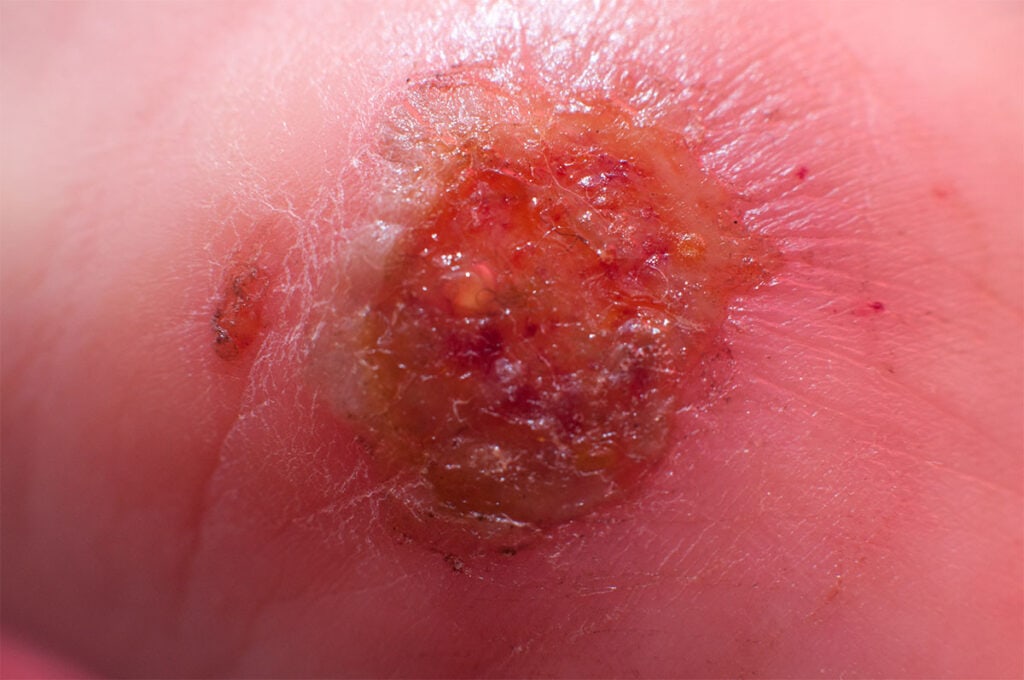
The following are the most common signs and symptoms of cellulitis:
- Skin Rashes and Redness
- Blisters and Bruises
- Pain and Tenderness at the Source
- Swelling of the Skin
- Aches and Chills
- Weakness and Fatigue
- Headache and Fever
An open skin wound that is infected is contagious through direct contact with another individual. Thus, it is important to have the area of infection covered, and any healthcare worker assessing the area should be using precautions to prevent the spread of the infection to others.
Cellulitis needs to address by a medical professional at the earliest opportunity to achieve the best outcome. Time is of the essence when it comes to treating, managing, and eradicating cellulitis.
When left untreated, complications likely to arise include severe tissue damage, internal organ damage, septic shock, amputation, and in rare instances, death.
Risk Factors for Cellulitis
While cellulitis can affect anyone, there are several risk factors associated with its development. Such risk factors include poor immunity, family history of cellulitis, obesity, diabetes, vascular disease, personal history of skin conditions, and injury.
To mitigate such risk factors, it’s important to make every effort to take care of your skin health and your overall health.
Treatments and Preventative Measures
Treating cellulitis infection involves treatment with appropriate antibiotics for the first 7-10 days after the first identified symptoms. Antibiotics typically alleviate symptoms and succeed in returning the patient to full health.
Should the infection persist, a longer regimen of antibiotics may be prescribed. In some cases, the infectious area can be cultured, especially if there is an open wound. Failure of antibiotic treatment may mean that the particular bacteria is resistant to the antibiotic. If this is the case, it is imperative to perform laboratory testing to identify which antibiotic can kill the bacteria. Then the curative antibiotic regimen can be employed to treat the cellulitis.
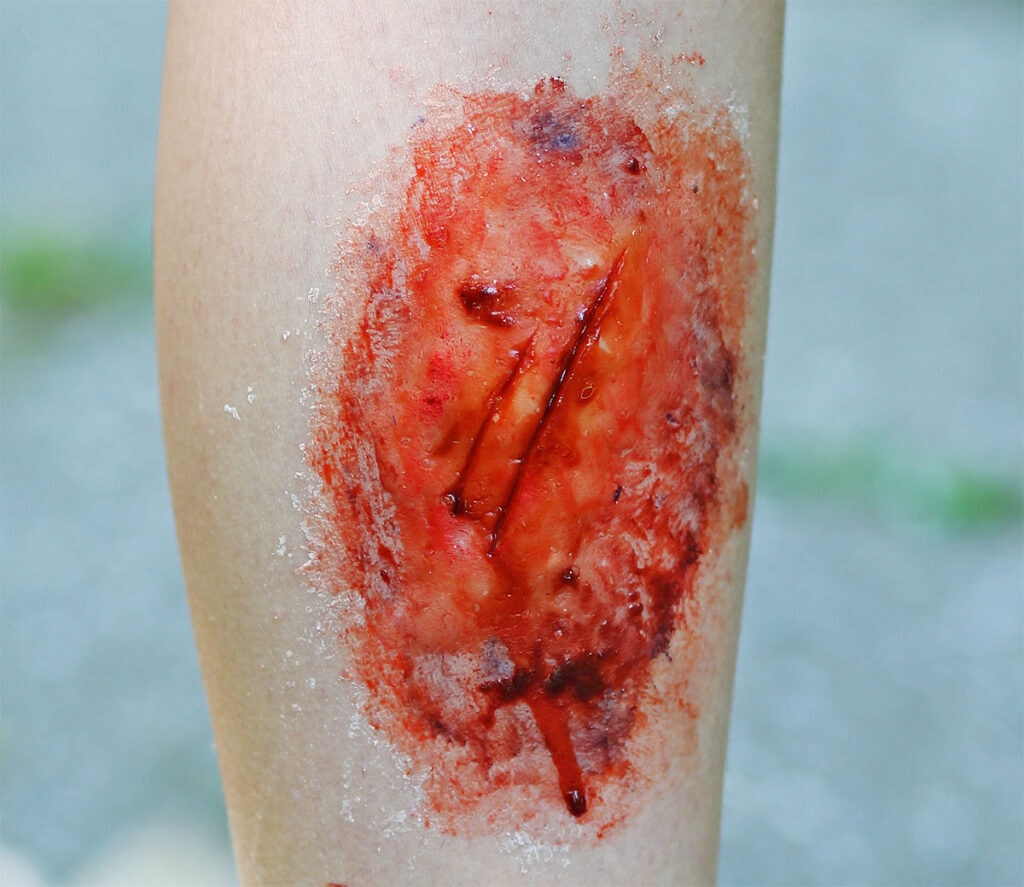
In some cases, an abscess can develop in the area of cellulitis, and surgical drainage may be required to treat the infection. One of the advanced treatments for poorly healing skin wounds that were caused by cellulitis is the wound vac. This device is a negative pressure dressing that has been extremely beneficial in healing such wounds.
Final Thoughts
Cellulitis is typically a mild skin infection that may be self-limiting or may require routine antibiotic treatment. Although it is a condition that can become severe and lead to life-threatening complications, it usually has a positive outlook.
The best outcomes result from timely intervention by a medical professional and effective treatment of the infection.




